By Heidi Smith, Contributor
It was Ash Wednesday, 2017. Fred Friedman and his wife, Kathy, remember it well.
As observant Catholics, the Minnesota snowbirds were fasting and reflecting. That morning, Fred and a neighbor had enjoyed a walk on Venice beach. Later, as Fred was trouble-shooting a malfunctioning TV in the bedroom, he suddenly felt dizzy and nauseous. There was a loud screeching noise in his ears.
“I thought the screeching was the TV somehow. I was so dizzy, I went to lie down on the bed, and yelled for my wife,” recalled Fred, now 72 years old.
“I knew he was calling me, but I couldn’t understand him,” Kathy said. “I thought he was joking around – talking funny.”
She quickly realized something was very wrong, and dialed 9-1-1.
The couple’s story of the next 72 hours shows how challenging it can be to diagnose stroke and how the speedy intervention of the stroke team at Venice Regional Bayfront Health can make all the difference in a survivor’s outcome.

Stroke Team Dives into Action
A call to 9-1-1 brought an EMS crew who put him through the standard tests for stroke and heart attack. Sarasota County Fire Department’s Emergency Medical Services team could see Fred symptoms, including a drooping face. They quickly transported him to Venice Regional, notifying the hospitals Emergency Department they were on the way with a possible stroke victim.
Venice Regional received an advanced certification as a primary stroke center by The Joint commission for eleven years in a row and has earned the highest possible rating from the American Heart Association’s Get with the Guidelines Program. Additionally, the hospital has interventional radiologists on call around the clock, which goes beyond the usual parameters for a primary stroke center.
Based on the heads up from EMS, the hospital’s Emergency Department, led by Medical Director Scott Fell, D.O., alerted the stroke team before Fred’s arrival. The team includes a neurologist, EKG technician, radiology department, medical lab, interventional radiology team, nursing and transport staff.
The neurologist on call was Tonya Stephenson, M.D., a board-certified clinical neurologist with Gulf Coast Neurology Associates. Dr. Stephenson is on the medical staff at Venice Regional, directs the stroke team, and serves on the hospital’s Board of Trustees.
“I remember Dr. Stephenson striding into the room where I was with Fred,” Kathy recalls. “She was wearing tennis shoes and she seemed to run everywhere she went. That really stuck in my mind – how focused she was on getting everything done quickly. How in charge she was.”
“The saying in stroke care is ‘time is brain,’” Dr. Stephenson explained. “When a large blood vessel in the brain is obstructed by a clot, nearly two million neurons in the brain can die each minute. A delay in treatment can be fatal or dramatically affect a patient’s ability to recover. The more brain we can protect from harm, the better the chance for undamaged parts of the brain to take over functions of areas damaged by a clot.”
Fred’s symptoms indicated a stroke. Next the team had to confirm whether it was a clot or a hemorrhage (bleeding). The treatment for a clot is usually a clot-busting medication, which dramatically thins the blood. If the medication is used when a patient is hemorrhaging, the result could be catastrophic, Dr. Stephenson explained.
One of the tests Dr. Stephenson needed to perform required injecting radiologic dye. Laboratory tests can be used to determine whether the patient’s kidneys can tolerate the dye. The Friedmans had established a relationship with a local primary care doctor – Zenobio Aguila, M.D., from Gulf Coast Medical Group – to consult during their annual winter stays in Venice.
That foresight now came into play.
“Fortunately, Mr. Friedman had very recently been to his local primary care physician who had ordered routine blood tests. Since his physician is in one of our affiliated Gulf Coast Medical Group practices, I was able to access the patient’s lab reports immediately through the computer network, which saved us valuable time and reassured us that the dye would not cause harm,” Dr. Stephenson said.
Clot-busting Drug Does Its Job
Diagnostic tests confirmed that Fred did not have a hemorrhage, which could have required neurosurgery. Nor was a large blood vessel obstructed, which could have required interventional radiology to extract the clot. Instead, Fred received an injection of alteplase, the clot-busting drug.
The nursing team watched Fred closely while the medicine did its work. Within minutes, Fred’s symptoms began to subside. His face muscles went back to normal, his speech normalized, and the double-vision he was experiencing resolved.
Fred was moved to the ICU where he stayed overnight with careful monitoring by the nursing team, Dr. Stephenson, and the critical care physicians dedicated to Venice Regional’s critical care units. Dr. Aguila, his primary care physician, also checked on Fred’s progress.
The next day, Fred received an MRI scan that confirmed clot damage in three small areas of the brain. With Fred’s condition stable and continuing to improve, he was moved to a room on the general neurology floor. He received visits from therapists for physical, occupational and speech therapy.
Because the MRI confirmed stroke from clots, the team called on Steven “Brad” Shoemaker, M.D., FACC, a board-certified interventional cardiologist at Gulf Coast Medical Group Regional Cardiac & Vascular Associates in Venice. Dr. Shoemaker conducted another test to look for clotting at the back of Fred’s heart.
The test didn’t reveal a clot but did show a small hole in Fred’s heart, confirming that Fred needed to be on a blood thinning medication. The test’s findings, combined with the stroke, indicated that Fred’s heartbeat should be monitored for irregularities. Dr. Shoemaker implanted a heartbeat monitor in Fred’s chest. The device is monitored remotely via the patient’s phone.
On the third day after arriving at the Emergency Department as a stroke alert, Fred went home.
“We have to say that the care I received at Venice Regional couldn’t have been better,” Fred said. “The care was out of this world. The emergency room, Dr. Stephenson, the family doctor. I couldn’t believe (Dr. Aguila) appeared at the ICU at 9 p.m., sat down and talked with me. ‘Are you okay? How did it go?’ That was a real standout for me.”
“Our son and his wife are nurse anesthetists, and they were scheduled to come to Venice for a visit when this happened,” Kathy related. “They came to the ICU and talked with the hospital caregivers. They were so satisfied with the care Fred was getting. It was reassuring to have medical professionals in the family telling us he was getting good care.”
Three years after the stroke, Fred takes a blood thinner and a blood pressure medication daily. He visits his Venice doctors each year during the couple’s winter stay in Florida.
“When we decided to stay in Venice for several months each year, we thought it was important to establish a relationship with a doctor who would know us if anything happened,” Fred explained. “In hindsight, that was one of the smartest decisions we’ve made. Gulf Coast Medical Group and Venice Regional took incredibly good care of me. It’s as good or better than any hospital I know.”
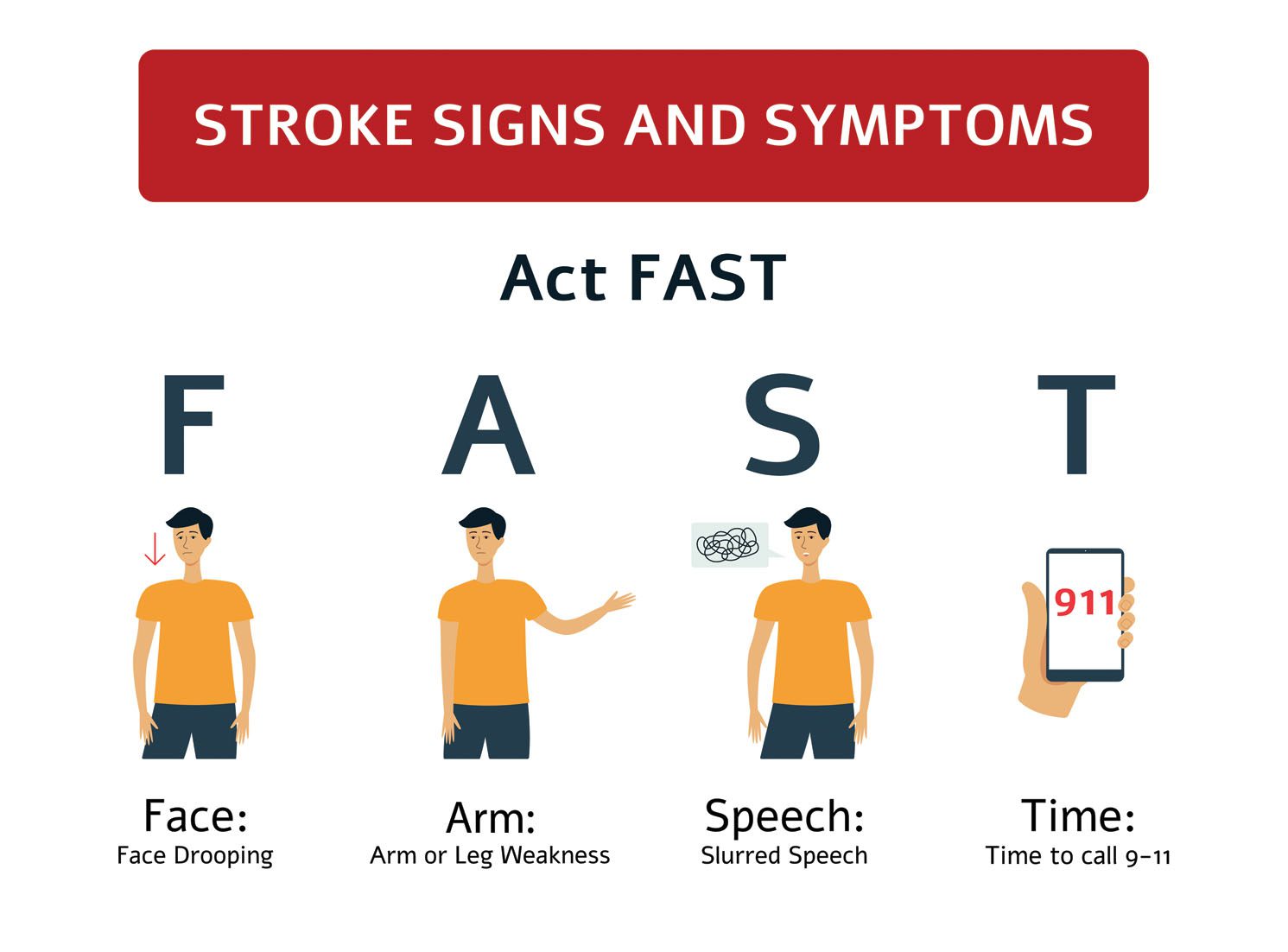
Know the signs: Spot a stroke F.A.S.T.
FACE DROOPING – Does one side of the face droop or is it numb? Ask the person to smile.
ARM WEAKNESS – Is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward?
SPEECH DIFFICULTY – Is speech slurred, are they unable to speak, or are they hard to understand? Ask the person to repeat a simple sentence, like “the sky is blue.” Is the sentence repeated correctly?
TIME TO CALL 9-1-1 – If the person shows any of these symptoms, even if the symptoms go away, call 9-1-1 and get them to the hospital immediately.
Source: American Heart Association | heart.org
Scott Fell, D.O., Medical Director of the Venice Regional Emergency Department team that launched the stroke alert for Fred Friedman.
Tonya Stephenson, M.D., a board-certified clinical neurologist with Gulf Coast Neurology Associates, leads Venice Regional’s stroke team.
Steven “Brad” Shoemaker, M.D., FACC, a board-certified interventional cardiologist with Regional Cardiac & Vascular Associates in Venice, consulted with the stroke team regarding Fred’s heart.
Zenobio Aguila, M.D., with Gulf Coast Medical Group, is the Friedmans’ primary care physician in Venice.
Venice Regional Bayfront Health
Call 941-488-1906 or visit
VeniceRegional.com
 Southwest Florida's Health and Wellness Magazine Health and Wellness Articles
Southwest Florida's Health and Wellness Magazine Health and Wellness Articles

