By Debra K. Brinker, RN
The popularity of regenerative, non-surgical treatments for osteoarthritis has grown in recent years and with good reason. People want options that are less invasive, do not require anesthesia or a hospital stay, and that have successful long-term results. Being diagnosed with osteoarthritis no longer has to mean giving up leisure activities and signing up for joint replacement surgery. Regenerative options can regrow cartilage and restore degenerated tissue, so that decreased mobility and chronic joint pain from arthritis become a thing of the past, along with some other outdated treatment options.
Why regenerative options make sense
Trace the process of osteoarthritis all the way back to the beginning. It is not just a disease of aging. An original injury to the soft tissue (such as ligaments, tendons, or other articular surfaces) whether through athletics, trauma, or insufficient recovery time, can result in weakness of the tissue. This creates imbalances and instability of the joint. The instability is part of the development of arthritis, occurring within a few years with severe injuries, or over decades when the injury is less severe. Since soft tissue is mainly responsible for the smooth movement necessary in the motion of the joint, when abnormal forces are placed on them, injury occurs that disrupts the balance between normal motion and instability. The disrupted balance in motion causes an uneven weight distribution inside the joint, with joint surfaces rubbing roughly and breaking down articular cartilage, limiting joint function, causing bone loss and eventually leading to the bony overgrowth of osteoarthritis. This is where the painful process begins.
Regenerative medicine aims to address the original soft tissue weakness or degeneration, to strengthen and repair these areas within the joint. By triggering the body to repair itself, cartilage can regrow naturally and the joint can stabilize, thereby resulting in diminished pain.
Cortisone injections and NSAIDs are not regenerative
Did you know that nonsteroidal anti-inflammatory drugs (NSAIDs) are among the most commonly used drugs in the world for the treatment of arthritis? Yet, one of the documented but lesser known long-term side effects of NSAIDs is their negative impact on articular cartilage. [See Figure] In essence, they accelerate the very disease for which they are most often used and prescribed. [See Figure 1]
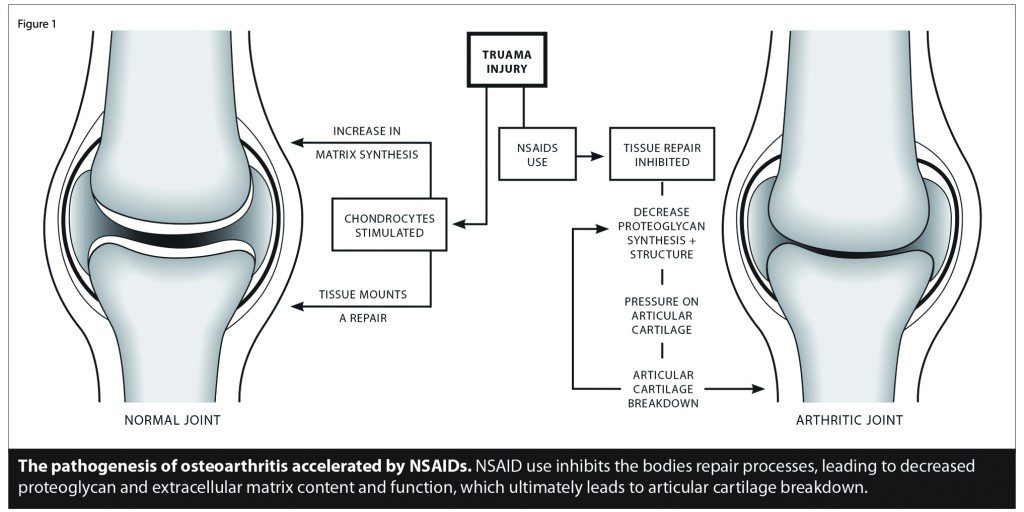

Corticosteroid injection is another common treatment for osteoarthritis with deleterious effects on the articular cartilage. Corticosteroids cause the cartilage to become thin, shredded, fibrillated, ulcerated, eroded, and ultimately destroyed, retarding and preventing its ability to repair. [See Figure 2]
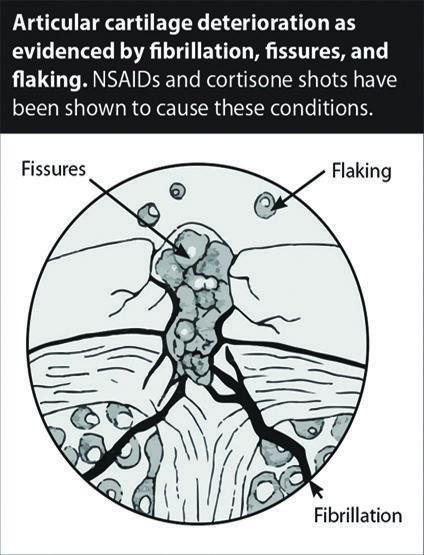

Since the hallmark feature of osteoarthritis is the breakdown in the articular cartilage of joints, further breaking down of the cartilage and accelerating the arthritic process by means of corticosteroid medications is not in any way reparative. This is why corticosteroid injections to a given joint are not to be performed more than three to four times per year, because of concern about the possible development of progressive cartilage damage through repeated injection in the weight-bearing joints.
Other treatments such as hyaluronic acid (viscosupplementation), exercise, physical therapy and lifestyle modifications are helpful at decreasing symptoms and improving mobility, but they do not repair the source of the problem or reverse the disease.
Prolotherapy – the regenerative option for osteoarthritisDegenerative conditions like arthritis need regeneration. The regenerative injection treatment used to repair the joint and to support a pro-chondrogenic (cartilage forming) environment is known as Prolotherapy. It involves the injections of natural substances into the degenerated areas to stimulate healing. It restarts the repair mechanisms in tissues that have lost the ability to repair on their own. This regenerative therapy has been found effective for the treatment of ligament and tendon injuries, and has a long history of use in osteoarthritis.
Stem cell therapy – Prolotherapy using your own cells
Another therapeutic strategy of this type is the injection of an autologous stem cell preparation. These cells from a person’s own fat or bone marrow can be injected directly into the damaged joint to accelerate the healing process in more severe cases of arthritis, in addition to comprehensively treating the surrounding soft tissues.
Cartilage improvement
The articular cartilage destruction is easily documented via standard X-ray. In the same way, improvement with Prolotherapy can also be documented by viewing X-ray changes. [See Figure 3]
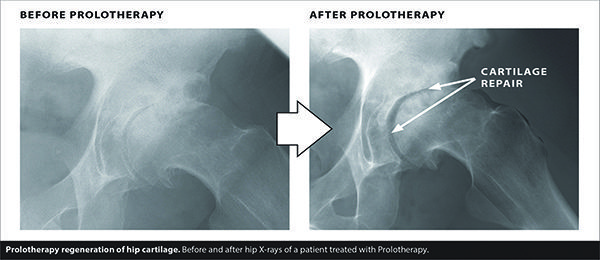

Prolotherapy, with or without the use of a person’s own stem cells, can be utilized to treat and restore most of the degenerated structures as well as the functioning of the joint. Even the majority of bone-on-bone osteoarthritis cases can be helped without the need for surgery. Post-surgical pain cases are also typically still candidates for regenerative options like Prolotherapy or Stem Cell Therapy. Whether in the early or later stages, the regenerative options for arthritis pain are better than ever.
Prolotherapy Specialists
CaringMedical.com
239-303-4546
with locations in Fort Myers and Chicagoland
 Southwest Florida's Health and Wellness Magazine Health and Wellness Articles
Southwest Florida's Health and Wellness Magazine Health and Wellness Articles

