Have you suffered a head or neck injury that has left you with chronic pain and debilitating, baffling symptoms that continue to worsen? Finding a specialist in cervical instability may provide answers.
Cervical instability occurs when the ligaments are lax and elongated from injury, allowing for an inefficient protective barrier. The cervical vertebrae are held in proper position by ligaments, helping to protect the spinal cord, brain stem, and nervous system from excess movement in the cervical spine. Damage to these soft tissue structures of the cervical spine can cause many more problems than just pain in the neck.
Cervical instability can provoke irritation of both the vertebral and sympathetic nerves. Damage to ligaments and ensuing irritation to the surrounding nerve endings may alter the firing patterns from these nerve endings, which may cause increased activation of the sympathetic nervous system. Even minor damage to ligaments can cause an over-stimulation of the sympathetic nervous
system. (See Figure 1.)
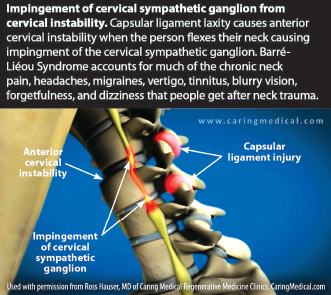

Symptoms of cervical instability
When the capsular ligaments of the neck become unstable, several things occur. For example, instability in the lower cervical spine (C3-C7) can cause muscle spasms, crepitation, and/or paresthesias in addition to chronic neck pain. Instability of the upper cervical spine (C0-C2) can cause numerous symptoms including, but not limited to, nerve irritation and vertebrobasilar insufficiency (VBI) with its associated symptoms of neck pain, headaches/migraines, dizziness, drop attacks, vertigo, difficulty swallowing and/or speaking, and auditory and visual disturbances. (See Figure 2.)
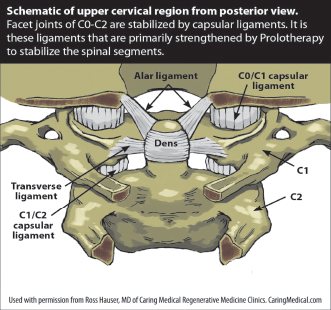

Symptoms from cervical instability can occur even after time has lapsed post-trauma, because the spine is destabilized. The destabilization causes aggressive, accelerated degeneration of the cervical spine affected by the trauma. Destabilization of the cervical spine can be accompanied by severe neurological sequelae such as those seen in instances of Post-Concussion Syndrome (PCS).
Post-concussion symptoms frequently occur following a concussion or mild traumatic brain injury (MTBI). Symptoms can include headaches, chronic neck pain, difficulty with concentration, sleep disturbance, irritability, memory deficits, sensitivity to noise, dizziness, vertigo, blurred vision, anxiety and depression. Symptoms notably similar to those of cervical instability. When this cluster of symptoms persists, the condition is then called Post-Concussion Syndrome. PCS symptoms can range in severity from being slightly annoying to becoming an overwhelming disability. In fact, symptoms have been reported to persist for 15 years or more after the injury. (See Figure 3.)
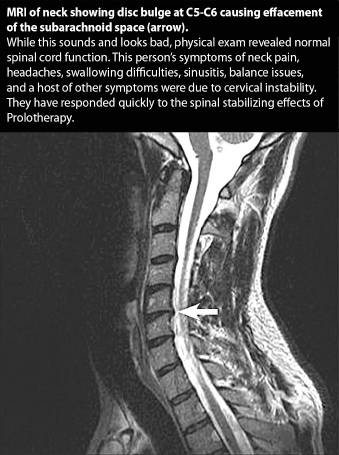

PCS, Cervical Instability and the Autonomic Nervous System
Due to the non-specificity of the symptoms of PCS, treatment can be complex. However, it is important to take into account the structures that may have been injured as a result of the jarring motion of the head.
The acceleration-deceleration forces involved in the trauma do not just affect the brain, but also create a significant whiplash injury to the neck and the base of the skull. Within these areas lies the brainstem, an area of the brain that controls our balance and
coordination, and supplies nerves to the muscles that control the eyes, ears, face, and portions of our autonomic nervous system (ANS).
The autonomic nervous system controls the bodily processes that occur automatically in the body, including breathing, heart rate, saliva formation, digestion, pain control, and of course, blood flow. Those with refractory PCS have a dysfunction of the ANS, as their physiologic functions fail to return to normal. A head injury resulting from a twisting mechanism or direct trauma to the upper cervical/posterior skull region may damage this ANS regulation.
Regenerative Therapy Treatments for Post-Concussion Syndrome Caused by Cervical Instability
The cervical spine should be carefully assessed for tenderness, spasm, and range of motion. If cervical instability is diagnosed, treatment would involve correcting the alignment and stabilizing the cervical spine. This can be accomplished with Regenerative Medicine treatment, such as Prolotherapy.
Prolotherapy injections reduce the excessive flexion and extension translation of the cervical spine. It does so by stimulating the repair of damaged structures, such as the ligaments of the cervical vertebrae, and the occipital and sub-occipital regions. (See Figure 4.)
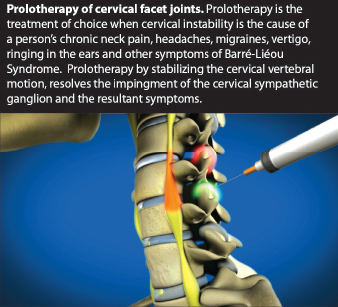

This regenerative injection therapy can provide hope and long-lasting, positive therapeutic relief from persistent symptoms associated with Post-Concussion Syndrome caused by cervical instability. Information and research on Prolotherapy for cervical spine conditions is available at AboutProlotherapy.com.
Prolotherapy Specialists:
Ross A. Hauser, MD.
Danielle R. Steilen. MMS, PA-C
Timothy L. Speciale, DO
239-303-4546
www.CaringMedical.com
 Southwest Florida's Health and Wellness Magazine Health and Wellness Articles
Southwest Florida's Health and Wellness Magazine Health and Wellness Articles

