By Debra K. Brinker, RN
Regenerative Medicine treatments provide an excellent option for patients suffering from a variety of symptoms that are due to cervical spine instability. Unfortunately, when cervical instability goes undiagnosed, patients can find themselves seeing numerous specialists and starting different medications that treat the symptoms but fail to fix the true underlying problem. Having a better understanding of the cervical spine, what symptoms are directly related to cervical instability, and how instability can be diagnosed and treated, can save a lot of time and help patients get back to an active and pain-free life.
Cervical Spine
The cervical vertebrae are held in proper position by ligaments, helping to protect the spinal cord, brain stem, and nervous system from excess movement. When the ligaments become lax and elongated due to an injury (such as whiplash or head injury)
or collagen disorder, cervical instability occurs. This may initially be perceived as head and neck pain, spinal clicking, and neck weakness. Cervical instability can provoke irritation of both the vertebral and sympathetic nerves. (See Figure 1.) Damage to ligaments and ensuing irritation to the surrounding nerve endings may alter the firing patterns from these nerve endings, which may cause increased activation of the sympathetic nervous system.
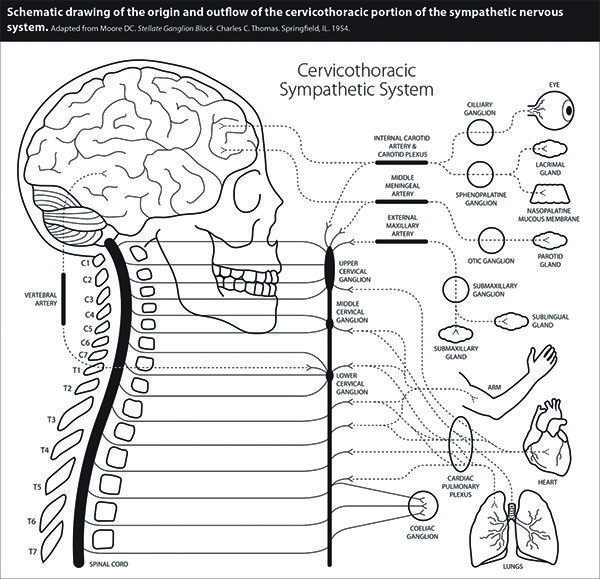

One condition that may develop due to this overactive state is dysautonomia which refers to problems of or dysfunction of the autonomic nervous system. The autonomic nervous system (ANS) is made up of nerves that control the automatic functions throughout the body. It is the master regulator, controlling heart rate, blood pressure, temperature, respiration, sweating, digestion and other vital functions. These systems operate without consciously thinking about them, because the ANS provides the connection between them and the brain. For this reason, when individuals suffer from dysautonomia, they often exhibit numerous maladies and symptoms. (See Figure 2.)


Postural tachycardia syndrome (POTS)
POTS is the most common form of dysautonomia with symptoms that manifest with the body’s inability to make the necessary adjustments to counteract gravity when standing up. Excessive heart rate increments upon standing is the defining symptom of POTS and is characterized by a marked rise of 30 beats per minute or greater within 10 minutes of standing from supine, or greater than 120 bpm while upright, and occurring in the absence of other chronic debilitating disorders. Tachycardia is often accompanied by a mild decrease in blood pressure. Sympathetic overactivity causes the tachycardia, mild hypotension, with brain and other organ hypoperfusion causing a host of other symptoms, which may include pre-syncope, syncope, dizziness, palpitations, headache, fatigue, bladder, and gastrointestinal (GI) symptoms.
Dysautonomia and Joint Instability Disorders
POTS is frequently associated with hypermobile conditions, such as Joint Hypermobility Syndrome (JHS) and Ehlers-Danlos Syndrome (EDS). Joint hypermobility is a condition where there is an increased range of joint movement due to a variant of collagen. JHS is a chronically disabling disorder manifested as widespread pain, fatigue, multiple soft tissue lesions and fragility of skin and supportive connective tissues, along with the aforementioned autonomic dysfunctions. Ehlers-Danlos Syndrome (EDS) involves the presence of joint hypermobility as well as other musculoskeletal and extra-articular connective tissue difficulties.
Upper cervical instability
The upper cervical spine (C1-C2) has a unique anatomical relationship with the vertebral arteries. When the vertebrae are unstable, the excessive and abnormal movements can alter vertebral arterial flow. Proper blood flow in the vertebral arteries is crucial because these arteries travel up to form the basilar artery at the brainstem and provide circulation to the posterior half of the brain. When this blood supply is insufficient, Vertebrobasilar Insufficiency (VBI) can develop and cause symptoms, such as neck pain, headaches/migraines, dizziness, drop attacks, vertigo, difficulty swallowing and/or speaking, and auditory and visual disturbances.
Treatment for improved cervical spine stability
Sympathetic stimulation can occur from any ligament or tendon injury or elongation. Instability continues to worsen if it is not stopped and the joints stabilized. (See Figure 3.) An exciting technology for patients who have been chasing symptoms and suspect that spinal or joint instability may be the culprit is Digital Motion X-ray (DMX). Unlike an MRI or static x-ray, DMX is like a movie of the joints going through their full range of motion. It picks up what other imaging can miss, especially when it comes to symptoms that occur when the head, neck, or other area is moved in a certain way.
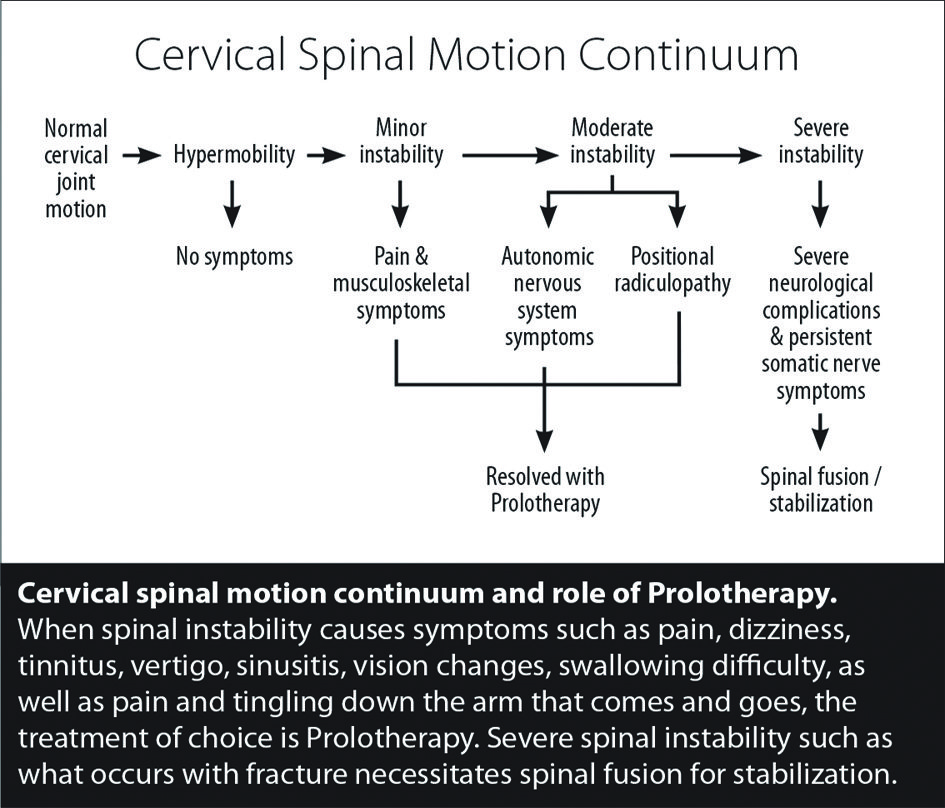

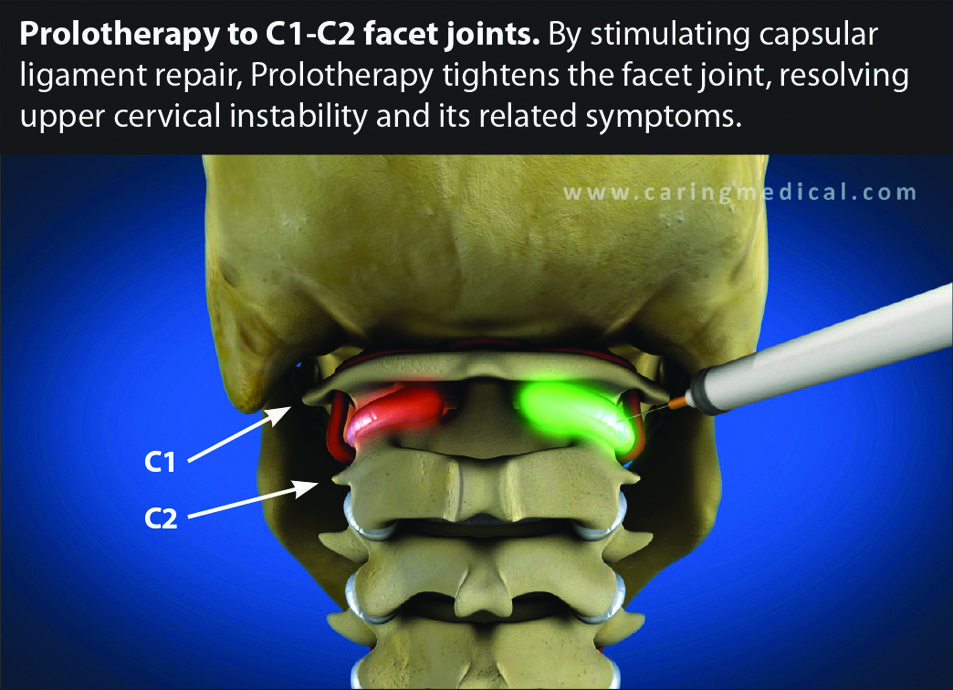
Regenerative treatments involve stimulating the body to repair, strengthen, and tighten the ligaments that hold the cervical vertebrae in proper alignment for movement of the head and neck. (Figure 4.) The use of Comprehensive Prolotherapy provides great hope to those with hypermobility because it is designed to successfully treat the ligament laxity/cervical instability and provide an alternative to cervical fusion surgery.

Regenerative Medicine Specialists
CaringMedical.com
239-303-4546
with locations in Fort Myers and Chicagoland
 Southwest Florida's Health and Wellness Magazine Health and Wellness Articles
Southwest Florida's Health and Wellness Magazine Health and Wellness Articles

